For any medical student, electives abroad provide the best chance to gain experience by working with a range of cases. Some of these cases you’ll have seen at home, but will be presented at more advanced stages in the developing world. Others will be totally unfamiliar to you.
Below, we’ve assessed the conditions most prevalent in the destinations we work in, and the factors that contribute to their pervasiveness. This will give you a clear idea of what you’ll be facing firsthand—a vital part of preparing for your medical elective overseas. What’s more, a deeper knowledge of the healthcare landscape will allow you to set aims and objectives that are realistic and achievable, whatever your destination.
Sri Lanka
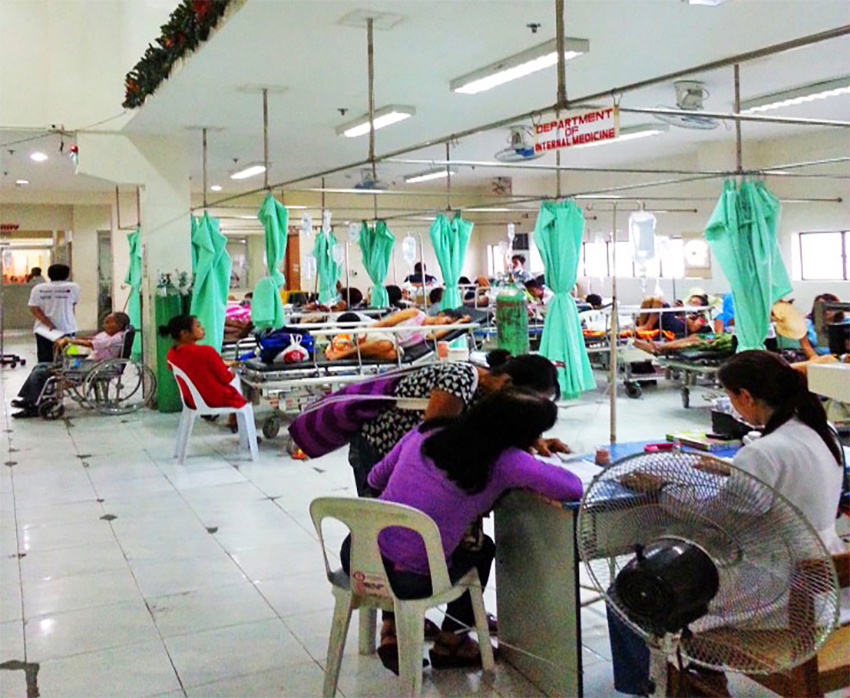
Sri Lanka’s high life expectancy, literacy rates, free healthcare, and free education are somewhat rare for a developing country. It’s healthcare system in particular has developed phenomenally over the past decade.
Having said that, cases of TB, Influenza, and Pneumonia are commonplace, as well as tropical infectious diseases like malaria and chikungunya. Like malaria, chikungunya is a mosquito-borne disease. Unlike malaria, symptoms of chikungunya include muscle pain and joint pain, and there is no cure, only pain management. If left untreated, the sufferer’s posture can become stooped. You’re very likely to come across chikungunya in our partner hospital, where you’ll observe and potentially assist specialists managing joint pain using anti-pyretics, optimal analgesics, and fluids. Gaining experience with these treatments in a low-resource environment will go towards the new skills you’ll learn on a medical elective here.
Another prevalent clinical issue in rural Sri Lanka is attempted suicide and deliberate self-harm. Although the rate of completed suicides in Sri Lanka has fallen since 1995, hospital admissions for non-fatal or attempted self-poisoning have increased in recent years. (BMC Public Health). Many use pharmaceutical drugs or pesticides as poison. In a study taken at a Teaching Hospital in Sri Lanka, qualitative interviews with those who self-poisoned revealed a multitude of motives. These included an inability to face feelings of shame, distress and emotional pain, physical pain, and anger. (BMC Public Health). It is also thought that its prevalence in young people is partly due to the high level of education they receive, whilst also living amongst poverty and limited resources. You may well encounter those affected by suicidal thoughts or self-harm on your elective, and an understanding of the condition’s pervasiveness—as well as the cultural pressures that motivate the aforementioned individuals—will help prepare you.
Asthma is a common non-communicable condition in Sri Lanka. So much so that the GAN (Global Asthma Network) has Sri Lanka marked as one of their ‘high prevalence’ countries. This is unsurprising considering asthma has increased in Sri Lanka by at least 50% in the last decade. Despite asthma being multifactorial, many attribute the increase in air pollution, irritants, and exposure to tobacco smoke as instrumental in the escalation of this particular lung disease. As such, it’s likely that you’ll encounter adults with bronchial asthma if you choose to work in the Outpatients Department of our partner hospital, assisting in the prescription of suitable drugs and treatment plans.
If you choose Sri Lanka for your placement, you’ll get involved with a diverse range of these cases, many of which could be presented at stages advanced far beyond what you’re used to at home. Don’t just take our word for it, however. Here’s what past students and professionals have had to say about their time in Sri Lanka’s wards and clinics:
‘My four weeks in Kandy was a rollercoaster of highlights, from the little paediatric patients who had a smile for me each morning, to my first experience of watching a Cardiothoracic Surgeon hold a beating human heart in confident hands.’ - Edward Spraggon, Medicine, Kandy.
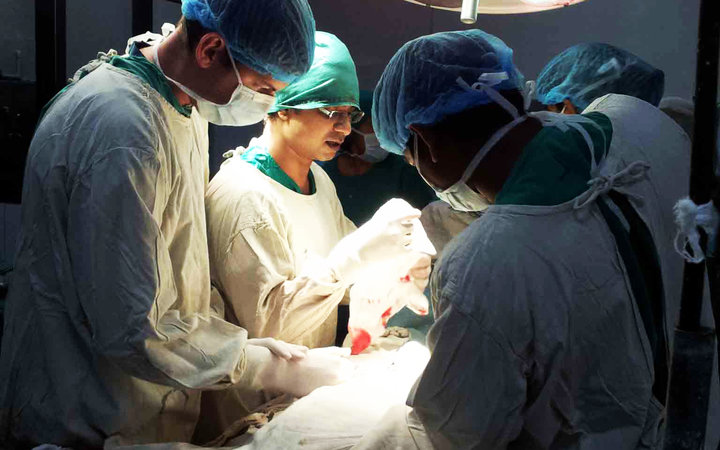
‘Seeing theatre in Sri Lanka really is an experience not to be missed! [...] Equipment is wrapped in material, medicines are kept in jam jars, and several operations take place in the same theatre simultaneously — all the while the next patients lie in a queue of trolleys, watching everything happening.’ Rebecca Mccauley, Medicine, Kandy.
THE PHILIPPINES
For the proactive medical student, electives abroad grant the opportunity to immerse oneself not only with unfamiliar conditions, but familiar ones, too. The difference you’ll find in addressing the latter is their social, cultural, and economic contexts; something you’ll be able to explore more deeply should you decide to undertake your medical elective in The Philippines.
The World Health Organization reports that the top cause of mortality in The Philippines is Ischaemic heart disease, followed closely by strokes. Although you may be familiar with these to some extent, the number of cases you’re likely to come across in The Philippines will be considerably more than you’re probably used to.
The number of fatal cases of Ischaemic heart disease has increased dramatically in the last ten years across the whole population. This could be put this down to the change in diet The Philippines has seen as it continues to urbanise towards Western standards. For example, popular fast food chains and canned drinks manufacturers have poured billions of dollars into the national market. This could also be related to unprecedented cases of tooth decay—with approximately 87.4% of the current populace suffering from the condition)—but an increase in blood-pressure and cardiac-related diseases, too.
The volume and frequency of cases you’ll see in The Philippines, as well as the limited resources specialists have access too, will make for an eye-opening experience. Here’s what past student Ammar has to say about his placement in The Philippines:
‘This experience is something that I will never forget; it allowed me to grow in terms of my medical career, my personality, and perspective on life. I did many things that I never thought I was strong enough to do, overcoming my fears and learning to adapt to a new environment in a short period of time. I would definitely recommend other medical students participate in a Work the World placement.’ Amaar Marefi, Medicine, The Philippines.
Nepal

Despite cases of maternal mortality, respiratory infections, and diarrhoeal diseases decreasing over the last decade or so, Nepal’s most threatening conditions are infectious diseases like TB, typhoid, dengue fever, yellow fever, and hepatitis. This is largely due to bodies of stagnant or contaminated water, and the humid environment of Nepal—both of which contribute to conditions in which insects that carry these diseases can thrive.
You might also come across lesser known infectious diseases like Leptospirosis, which is transmitted through bacteria found in rodents. “Whenever there is a flooding, these bacteria get mixed with water and enter the human body through cuts in feet. Those working in fields are prone to the disease as they work [with] bare feet,” points out Dr Bastola, a doctor from Nepal. (The Himalayan Times) It’s encountering these sorts of diseases that will grant you a broader perspective of your field.
Another disease you’re likely to come across here is kidney disease. This is because the introduction of pesticides to agriculture has been known to contaminate rural water sources, resulting in an increase of kidney disease and subsequent transplants. This is largely due to the lack of education given to rural farmers, many of whom are unaware of pesticide types, safety precautions, and the hazards these chemicals can cause to both health and the environment when handled liberally or without adequate protection (JAE). “Though chemical control is being practiced by many farmers, many use harmful and expensive pesticides ignoring our recommendations,” affirms Bharat Prasad Upadhyay, an official at the country’s Crop Protection Department (IPS).
Diagnosing and treating these conditions will provide you with diverse experience, which will help you begin to form a well-rounded and compassionate medical ethic, as well as bolstering the basics of practice. Here’s what our students have experienced firsthand while on placement in Kathmandu:
‘As expected, I saw conditions less common in Australia and dominant in Nepal. The most striking was Tuberculosis. Whilst TB can be found in certain parts of northern Queensland, it definitely is not common in the Gold Coast, and as a communicable disease must be reported to the government. However, in Nepal, the predominant belief is that everyone has at least latent TB already, and thus very few precautions are taken to prevent its spread, even amongst healthcare workers. It was remarkable to see all the foreign medical elective students wearing their facemasks on the ward rounds, yet the Nepalese staff bare faced.’ - Progga Sasha, Kathmandu.
‘Both working in a local hospital and visiting an Ayurvedic hospital gave me two different experiences in this country. Witnessing the contrast between allopathic and homeopathic medicine opened my eyes to the challenges that traditional and nontraditional healthcare professionals may face.’ - David Dao, Kathmandu.
TANZANIA
As in many African countries, HIV/AIDS is a huge priority for healthcare professionals in Tanzania. Around 1.2 million of those aged 15 or over live with the virus, accounting for over 5% of the adult population. (This compares with around 0.2% of adults in the UK.) (Our Africa). Not only does this put a huge strain on Tanzania’s health care system, but the lack of available resources often cause complications when treating HIV positive patients.
The prevalence of HIV/AIDS in Tanzania is , in part, due to a lack of preventative sexual education, poverty, and gender inequality. Women tend to become infected earlier, because they are likely to have older partners and get married at a younger age. (Avert). They also experience difficulty in negotiating safer sex, due to pervasive gender inequality. As such, it’s likely that medical students in Tanzania will encounter HIV positive mothers, or mothers-to-be. You’ll learn exactly how HIV can be transmitted from mother to child during pregnancy, childbirth, and breastfeeding, and observe the proper use of antiretroviral treatment, which can reduce the risk of infant contraction by up to 40% (Avert).
For the ambitious medical student, electives abroad in this part of Africa bring the chance to work more closely with HIV patients, getting to grips with how the disease is diagnosed, treated, and prevented with limited resources. Should you take your elective in Dar es Salaam, you could choose to work in our partner hospital’s Internal Medicine Department amongst many others. Here, malaria, HIV, and cholera make up around 75% of all cases.
‘On the infectious diseases ward the pattern of presentations was very different to the UK. There were numerous cases of HIV and its sequelae, tuberculosis infections and one possible case of rabies. ’ Alice Hanton - Tanzania
Ghana
The variety and severity of cases you’ll be exposed to in Ghana will be a challenge you’ll reap a host of experiences from. According to the World Health Organization, the diseases most common in Ghana are those endemic to sub-Saharan African countries, particularly: cholera, typhoid, pulmonary tuberculosis, anthrax, pertussis, tetanus, hepatitis, trachoma, malaria, and HIV and schistosomiasis.
Malaria, in particular, is one of Ghana’s most prevalent diseases. According to UNICEF, it accounts for up to 25% of the deaths of children under the age of five, and is a large drain on the few resources the Ghana healthcare system has. There are many factors responsible for Malaria’s prevalence; in sub-Saharan Africa, the principal malaria mosquito, Anopheles gambiae, transmits malaria extremely efficiently. The most common type of parasite, Plasmodium falciparum, causes severe and potentially fatal disease. A lack of both resources and political stability has prevented the establishing of solid malaria control programs, worsening the situation.
Working with cases of malaria will not only give you the chance to glean insight into a totally unfamiliar disease, but open your eyes to the ways in which it’s treated locally. The way the condition affects the lives of those who carry it will also hit home.
For both medical professionals and medical students, electives abroad in Ghana have always proved to be eye-opening experiences:
‘I learnt a lot about malaria [...], which I had little clinical experience of before going to Ghana. Many patients present late in Ghana, so although it was often tough to see patients who were very ill and had a poor prognosis, it was an opportunity to see clinical signs I would never have seen at home.’ - Claire McGinn, Takoradi, Medicine.
‘Tropical diseases were disturbingly common. So, too, were patients presenting when their disease was already well advanced. You will see things here you won’t see in Australia.’ - Jessica Murray, Takoradi, Medicine.
‘I saw many interesting cases, which included snake bites, sickle-cell, seizures, HIV, malaria, sepsis, hypertension, diabetes, gastroenteritis, bone fractures, urinary retention, electric burns, gangrene, hernias, peritonitis, appendicitis, tuberculosis, typhoid fever, vessel occlusion crisis, leg ulcers, Kaposi’s Sarcoma, and Fallot's Tetralogy.’ - Melissa Fox, Takoradi.
WHAT NEXT?
It’s common knowledge that for medical students, electives abroad are the best way to learn new skills, broaden your mind, and better prepare yourself for a future in medicine. The incredible diversity you’ll be exposed to in any of our destinations has hopefully encouraged you to consider an overseas placement. You’ll gain unparalleled insight into varying healthcare systems, meet people from all walks of life, and grow into the professional you’re striving to become. Whether you’re interested in working in Tanzania’s HIV clinics, encountering pesticide-induced kidney disease in Sri Lanka, or tropical infectious diseases in Nepal, there’s extensive experience to be gained from taking your medical elective abroad with Work the World.
To speak with one of our elective experts, fill out the short enquiry form and we’ll be in touch. Read more about our medical electives abroad.

Start your journey
Start dreaming up your perfect overseas elective placement today by browsing our destinations below.
Start dreaming up your perfect overseas elective placement today by browsing our destinations below.