Dr Charlotte O'Byrne travelled to Iloilo in The Philippines for her medical elective between the fourth and fifth years of her medical degree. We interviewed her to see how it all started and asked her how her time overseas helped her get to where she is today.
 Joe: So let's start right at the beginning. What was it, if you can remember, that made you want to study medicine?
Joe: So let's start right at the beginning. What was it, if you can remember, that made you want to study medicine?
Charlotte: I know it’s a cliché, but it started at a young age.
I remember starting high school and having my first science lesson and loving it. I loved science more than any other subject and I was quite good at it. That’s probably where it all started.
I’ve also been a performer since I was young. I’ve always danced and been in musicals. In the end, I was torn between wanting to perform and loving science. But when I started thinking about medicine, I realised it put the communication and people skills I’d learned through performing together with the science.
I think I must have been 12 or 13 when I first formed thoughts of becoming a doctor.
Once I’d decided to pursue it, everything I did was working towards that goal.
You said you went through secondary school with becoming a doctor in mind. How did you get from there to studying medicine at Leeds?
I’m from Leeds, so it was close to home. That made the transition to university a bit easier.
The application process for a medical degree is gruelling. You get a lot of rejection, and a lot of it feels like luck. You won’t find anything out until the last minute. Your friends who aren’t aiming for medicine probably already have offers. You’re just waiting around having done all these interviews. It’s scary, and you just go to whichever university you get into.
 I got into Leeds and Newcastle, but I wanted to stay near home. And I loved Leeds at the open day, so I ended up staying there.
I got into Leeds and Newcastle, but I wanted to stay near home. And I loved Leeds at the open day, so I ended up staying there.
This is a broad question, but how was it, as an experience?
It was really good, I loved it. I had the best six years. I intercalated so that made it six as opposed to five.
And having the extra support of being close to home helped.
I was still independent and living away from home, but home was only ten mins away. I went back to eat roast dinners and get my laundry done. Or to cry with my mum when things were hard, which they were from time to time.
Did having that support alleviate any of the pressure of the study itself?
It did, it was really helpful. I knew it was going to be stressful, so I looked for ways to try and protect myself and look after my mental health.
Keeping up the performance side of things helped as well.
I choreographed five musicals while I was at uni. I started a medic’s dance society and that was tied in with an existing medic’s musical society, so I became the resident choreographer. I’m doing another one now even though I’m now a doctor, it’s a good outlet when you’re feeling stressed.
 As if you weren’t busy enough with your studies!
As if you weren’t busy enough with your studies!
It’s always had more pros than cons. It was beneficial for me, I ended up managing my time better, I felt less stressed, and I met students from the years above who helped me out.
It was a girl I met through society who told me about Work the World.
And what year were you in when you travelled with us?
I was between my intercalation year and my final year. At Leeds, you have to do your six-week elective in the summer before your final year. Because I’d taken a year out to do an extra degree between my fourth and final year, I travelled with Work the World between that extra degree and my final year.
An extra degree — impressive! What did you study?
I studied primary care. It was all about the world of general practice, outside of hospital medicine.
I enjoyed it. And it was good to take a ‘year out’. Because even though it was effectively undertaking a degree in the space of a year, it was chilled out compared to any year of medicine I’d done.
That might sound like a weird thing to say, but I think most people take the extra year as a ‘year out’. It lets you be a ‘normal’ student for a while.
 So it gave you a bit of a breather, in an unusual way?
So it gave you a bit of a breather, in an unusual way?
It did. And because I did that extra year, I had plenty of extra time to plan for my elective. If I’d done it after my fourth year, it would have been stressful, the fourth year being an intense year for a medical student. But instead, I had free days to plan things and get everything set up and ready.
That sounds sensible to me. Is that quite a common way of doing things?
It isn’t. It’s quite rare for someone to intercalate after the fourth year. Most people intercalate after the third year. I admit I was a bit late to the party with intercalations.
But intercalating after the fourth year seems to make a lot of sense. The bulk of your medical degree is out of the way, and you’ve got a year to catch your breath before heading into the final year.
Exactly. It was a bit of a fluke, but now I go around telling all the younger students that this is the way to do it. The fourth year is the hardest year, so having that out of the way means you can enjoy your final year.
I think you’re onto something there.
I’m flying the flag!
 You mentioned that you met another student who introduced you to Work the World. What was the timeline from when you learned about it, to landing in the country? What was that process like?
You mentioned that you met another student who introduced you to Work the World. What was the timeline from when you learned about it, to landing in the country? What was that process like?
So I saw my friend, Jenny, a lot at rehearsals. I spoke to her about how I didn’t know what I wanted to do for my elective. And I remembered seeing photos on Facebook of her in her elective. I remember thinking that she looked like she was having fun. I told Jenny that I wanted to go somewhere on my own. Lots of people in my year were going in big groups. There was a big group going to Sri Lanka, and a big group going to Australia.
I didn’t want to do that. I didn’t want to have to go where everyone else was going. I wanted to have more control over my own experience.
I didn’t do a gap year. I haven’t even been on many holidays. I’d not been in a position to properly travel before, so I was nervous. The whole idea terrified me. Initially, I didn’t think it was going to be an option for me.
So in my conversations with Jenny, I told her that I wanted to go on my own. I told her that I wanted to challenge myself, but that I was scared to go alone. I was worried I wouldn’t feel safe. I told her that I hadn’t travelled before, and had no idea how to go about organising it. How would I know everything was legit? I had lots of worries like that.
Jenny just said to me, “Well it sounds like you should do exactly what I did.”
 I thought that was a great idea. Someone I knew and trusted who had already had the experience was making a recommendation. She knew me well as a person, and her telling me that I’d be fine made a big difference.
I thought that was a great idea. Someone I knew and trusted who had already had the experience was making a recommendation. She knew me well as a person, and her telling me that I’d be fine made a big difference.
She showed me photos and told me about everything she’d done. We spoke about her hospital placement, but also about the fun travel stuff. It sounded like the combination I wanted.
I went on the Work the World website and it was all straightforward from there. Before I read about it, I thought I’d have to organise it all myself. But the website explained everything clearly.
So then I spoke to my mum and dad and told them that I had a really good feeling about this. I told them I was just going to go ahead and do it — I didn’t want to think about it too much in case I got nervous and changed my mind.
Well, the fact that we’re talking now implies that you made the right decision.
I did!
So you went ahead and booked on. After that, you must have gone through our pre-departure process, and then it’s time to go. How were you feeling at that stage?
Nervous.
It would be a total lie to say that I wasn’t. It would be more accurate to say that I was a mess.
The team were great at reassuring me, but that’s just who I was at the time.
Something that helped was MyTrip.
[MyTrip is Work the World’s elective placement planner.]
You have all the information you need right there in front of you — things you need to do, things you need to prepare. I felt better every time I ticked something off. There were times when I thought, “What have I not signed, not packed, not paid for?” Logging in and seeing it all done and laid out made that feeling go away.
I can’t tell you the number of times I loaded it up and looked at all the little green ticks that showed I’d already done everything I needed to do. It reassured me in a big way.
I also had calls and exchanged emails with the Work the World team. But there’s this one call you get before you go that’s particularly reassuring. You get all the logistics around what will happen when you arrive and where a member of the local Work the World team will be waiting for you when you arrive.
That’s one of the reasons we make all of our pre-departure services so comprehensive. It’s not like you’re popping to France for a weekend — you’re travelling across the world.
 So, before you know it you’re on the plane. Can you talk us through that first 24 hours?
So, before you know it you’re on the plane. Can you talk us through that first 24 hours?
The journey was an emotional one.
I said goodbye to my family at the airport and sobbed through security. I’m not sure what the staff thought of me.
I was so nervous. I was wondering what I’d done, thinking I should have stayed in Leeds. I was worried about getting there and being that person who stays in the house the whole time crying and missing home.
I didn’t want to be that person — I wanted to be able to justify having gone out there by having a good experience.
I sat next to a family on the flight. They noticed that I was struggling emotionally. I couldn’t sleep either. The mum of this family turned around and said “Where are you going?” And I told her all about it. She told me that what I was doing was amazing and that my mum will be proud. We were both sitting there chatting together on this flight.
Landing in Iloilo was about as surreal as you can imagine. I was relieved to have arrived, and this mum on the plane had been so nice to me. Then the business of the airport hit.
It was very different. It was so busy and seemed disorganised. The departure boards were just someone on a laptop with Powerpoint open connected to a screen.
 When I was waiting for my internal flight it was delayed. But there were no updates. We went way past the time it was due to leave but heard nothing. Hours seemed to go by and no one told us what was happening.
When I was waiting for my internal flight it was delayed. But there were no updates. We went way past the time it was due to leave but heard nothing. Hours seemed to go by and no one told us what was happening.
I remember looking around and thinking that if I asked for information, no one was going to understand what was saying. I thought I’d just sit in my corner by the gate and hope for the best.
And then I started worrying. Are the people on the other end even going to be there now that I’m so late and haven’t been in touch?
I decided to call one of the numbers I’d been given for one of the people at the Work the World house. I got through and told them I was in Manila airport and that I was stuck. And straight away they told me not to worry and that someone would be there. They told me that everything was going to be fine. I felt a lot better. Then I finally got on the flight.
When I landed I was so relieved to be there. As soon as I walked out of the airport, there was someone in their blue Work the World T-shirt, standing exactly where I was told they’d be.
So we got into a taxi, and on the way the Work the World team member asked if there was anything I couldn’t eat. I told her I was allergic to coconuts and she immediately rang the kitchen at the Work the World house. She told them that I couldn’t eat coconut, and I thought “This is well organised!”
 It was early in the morning when we arrived at the house. But despite that, there was a meal laid out on the table for me. So I sat and had this meal, and then the team showed me around the house and where my room was. Then all the other students who were already in the house woke up.
It was early in the morning when we arrived at the house. But despite that, there was a meal laid out on the table for me. So I sat and had this meal, and then the team showed me around the house and where my room was. Then all the other students who were already in the house woke up.
What was that like?
It was a bit overwhelming at first. There was a group of 11 students from Belfast. They’d been there for four weeks and seemed settled. But then other students’d come in pairs. And there were a couple of people on their own, like me. They came from Australia, America, the Netherlands, the UK… from all over the world.
By pure chance, two of the girls who were in my room were from Hull York Medical School (if you don’t know, that’s quite close to Leeds). We got on, and for the rest of the time, it kind of felt like I’d travelled there with them.
I think that because you’re in a shared room you have to get to know people. Sleeping in the same room, eating meals together and going to the hospital together — you quickly form bonds.
That morning we went on our local orientation with the Work the World team. I think there were about six of us starting on the same day. The team took us to the town hall, and we went up to the roof where we could see the whole city.
The team then took us for some traditional Filipino food. Food was something I worried about. I’m known in my family for being a fussy eater, but from that very first meal, I knew it would be fine and that I’d be able to eat everything.
One of the things we make a point about is that we’ll always cater to your dietary requirements regardless of what they are. So what sort of things were you eating in the house?
It was different every day. There was a board outside our room with the menu on it and every morning we’d pop out and check it. One of our favourites was an Oreo pudding that the catering team made on BBQ nights.
One night the team made a curry-style dish and it had coconut in it. I couldn’t eat it, so before they brought out everyone else’s food, they brought out five different plates and bowls of food that were just for me. They always went above and beyond if you had any requirements.
There were a couple of girls who could only eat Halal food, there was a vegan... There were people with specific dietary requirements, but the caterers always made amazing food.
So the other side of all this is the hospital placement. What were you feeling when you stepped into the hospital for the first time?
It was strange. We pulled up outside and it seemed like it was going to be quite a big place. From the outside, it seemed like it was going to be more modern than I imagined.
 Then we went inside. As we walked around the different areas, we saw that things weren’t as modern as the exterior. There were even cracks in the walls and the floors. They were struggling when it came to infrastructure.
Then we went inside. As we walked around the different areas, we saw that things weren’t as modern as the exterior. There were even cracks in the walls and the floors. They were struggling when it came to infrastructure.
We walked around the hospital and we saw things you’d never see back home. There were multiple patients per bed in some places. The obstetrics ward in particular, with up to three mothers and their babies in one bed.
That’s quite a first impression.
It is. I think it’s difficult to explain to people who haven’t been there. I saw straight away that I was wrong about a lot of the assumptions I’d made about what I was going to see.
We had a big orientation talk from the Chief Medical Officer in the hospital. And they just seemed to be so welcoming and so happy to have us there. They were so proud of their hospital.
I thought we were going to encounter more downtrodden people. I thought people were going to try to tell us how awful everything was for them. It was quite the opposite.
Staff were telling us about a new stroke ward that had opened and how proud they were of it.
When they spoke more about it, the only reason they’d been able to open this department was that they’d managed to acquire a big box of anticoagulants. They were out of date, but it was a way for them to help patients.
 They were just so proud of this ward. The whole time I couldn’t help thinking about how far behind it was compared to what we have in the UK.
They were just so proud of this ward. The whole time I couldn’t help thinking about how far behind it was compared to what we have in the UK.
So once you’d started the placement, what was the day-to-day like?
So we’d all get up and have breakfast together, then we’d travel to the hospital itself by ‘Jeepney’.
[A Jeepney - pictured - is a Jeep that has been converted into a sort of hop-on, hop-off public bus.]
They were so much fun, but they were hard to climb into. They had low ceilings so you nearly had to fold yourself in two to fit in!
When we arrived, we all went off to our separate departments.
I spent two weeks in anaesthetics, two weeks in paediatrics, and two weeks in OBG.
I started on anaesthetics. The doctors there were lovely. They involved us as much as we wanted to be involved. Though saying that if it was a procedure I wasn’t trained in and wouldn’t do to a British patient, I wasn’t going to do that to a patient in The Philippines.
Doing anaesthetics meant seeing a lot of surgery, and it couldn’t have been more different from home. The theatre rooms needed actual building work done to them, and that’s before you even start commenting on the medical equipment.
 But I was surprised by the level of surgery they were able to pull off there. I watched a craniotomy on a 7-year-old boy and they removed the top of his skull to try and remove a brain tumour. It was a last-ditch attempt to save the boy’s life. This is an operation we think very carefully about doing even back home.
But I was surprised by the level of surgery they were able to pull off there. I watched a craniotomy on a 7-year-old boy and they removed the top of his skull to try and remove a brain tumour. It was a last-ditch attempt to save the boy’s life. This is an operation we think very carefully about doing even back home.
During the operation, a fly came into the operating theatre and circled the boy’s exposed brain. The surgeon quickly put a sterile drape over the brain just before the fly landed on it. The other students and I chased this fly around the theatre with clipboards trying to swat it!
The surgeon then said, “That’s developing-world surgery for you!”
I bet that’s not something you learn in med school, is it?
You’re right!
This surgery went on for hours, as it would normally. But one of the key differences was that they didn’t have the kind of mechanical ventilators we have. The anaesthetist had to stand there and squeeze the bag. And if they didn’t squeeze the bag, the patient didn’t breathe. Nothing was automated.
The surgeons and anaesthetists were amazing. They wanted to teach us, so they talked through everything they did.
The anaesthetists took us out for drinks at the end of our third week, and it was nice to get to know them.
 They told us that they’d had the option to go and work in the better-funded private hospitals, but they wanted to train in a government hospital. It was interesting to hear that they were learning a lot more than their peers who were in private hospitals around the country.
They told us that they’d had the option to go and work in the better-funded private hospitals, but they wanted to train in a government hospital. It was interesting to hear that they were learning a lot more than their peers who were in private hospitals around the country.
So were there any particular cases that stick out in your mind? You’ve spoken about this craniotomy experience, but do any others spring to mind?
The ones that stick in my head, the ones I think about every day, are the ones I saw in the delivery rooms.
I still think about this particular case where a lady gave birth to a stillborn baby. The baby had a genetic condition that, back in the UK, we would have diagnosed with an antenatal scan. That mother would then be prepared for what her baby was going to be born with. But in The Philippines, they don’t have the antenatal care that we have. They don’t have the capacity for prenatal diagnosis.
So this baby was stillborn and they immediately took the baby away from the mother. She didn’t see her baby at all. The mum was expected to deal with it. Then they were quickly getting the mum out and getting the next woman in.
Fathers or birthing partners weren’t allowed in either, so she didn’t have anyone there to support her.
It was all quite challenging to observe.
 Why do you think this was the approach? Why do you think it differed so much from what you normally see in the UK?
Why do you think this was the approach? Why do you think it differed so much from what you normally see in the UK?
Having spent quite a bit of time out there with these people, I learned that death was thought about very differently over there.
It’s not that we find death more tragic in the UK, but for us, death seems ‘unnatural’ if we’re young, or the death is traumatic. Those kinds of deaths are far less common for us.
For example, it’s abnormal for someone young to die, especially a baby. Whereas in The Philippines, giving birth is a much riskier business, and you might not even get a baby at the end of it.
If you live in The Philippines and your relative gets hit by a car, you wouldn’t expect them to live. The expectation isn’t that you take them to the hospital and they get fixed. It’s that you take them to the hospital in a desperate attempt to hold on to them.
Death is more a part of their lives. That’s the impression I got anyway. The way they dealt with death was that it was already more of an expectation, and therefore they were more prepared for it.
There was one boy who was brought in by a hysterical parent. He had been bending down to pick up some coins off the floor and was hit by a car. The accident had almost taken his scalp off.
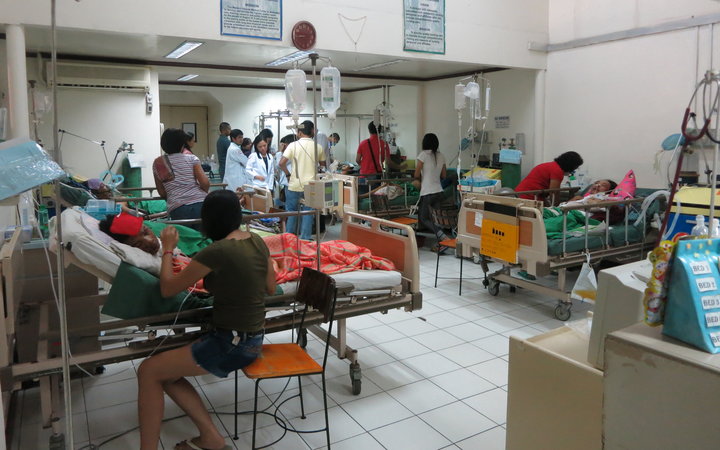 Then the money thing came up. This child needed surgery to stitch his scalp together. But the family didn’t have the money. In The Philippines, you have to pay upfront for treatment or it’s not going to happen.
Then the money thing came up. This child needed surgery to stitch his scalp together. But the family didn’t have the money. In The Philippines, you have to pay upfront for treatment or it’s not going to happen.
We’re talking a negligible amount of money — money we carry around in our pockets back home. I think that was the hardest thing to deal with out there.
How did you deal with it?
It was tough. It would have been easy to put our hands in our pockets and just hand over the money.
But you can’t do that. You can’t be that random Westerner who just so happens to be there on that particular day and play God. What about tomorrow when I’m not there and things have to go back to normal? If you do something like that you’re failing to understand the problem. You’re interfering with local people’s views on injury and healthcare and death, just because you wanted to be a hero.
My housemates and I talked about this a lot, and we concluded that it wasn’t something we felt comfortable doing. It goes back to that whole idea of ‘voluntourism’ where people think they can go out there and ‘make a difference’.
None of us saw ourselves as that sort of person. We were there to experience, and to try to understand things. We were there to learn about another culture and another system and then to take those lessons home. It was never about trying to save people.
 I think if you go out with the saviour mentality, you’re going to feel disappointed in reality.
I think if you go out with the saviour mentality, you’re going to feel disappointed in reality.
Words of wisdom to say the least. And we make this clear to everyone before they travel with us. I think you’re exactly right when you say that you’re going there for the experience and the understanding rather than to ‘save the world’ as it were.
Exactly. You’re simply not going to — it’s unrealistic. You’re going to see that this is how things are for people in many developing countries. This is their reality. It’s wrong to go there thinking that you’re going to save everyone when there are fundamental problems like a lack of funding.
I asked a doctor one day, “Why do you think it’s like this? What are the barriers to making this hospital better?”
He said to me, “You have to think about it as a hierarchy of needs.” He went on to explain that healthcare isn’t necessarily a government priority. First, they have to have security, and then they can work on developing infrastructure. Then you get hospital buildings that are fit for purpose, and then you think about staffing. Then you can start getting all the wonder drugs that we have back home. It sounds silly, but healthcare is a luxury over there.
 So, you had this life-changing experience in The Philippines.
So, you had this life-changing experience in The Philippines.
I did.
Then you came back to the UK and you said you were between your 5th and 6th years.
How did you approach that final year of your studies having had that experience?
So I think about it like this: I don’t like the sun, I don’t like being away from home, and I don’t like being on my own. But I had the time of my life in The Philippines. The placement, the house, the travelling — it was all amazing. I said yes to everything and pushed myself.
When I was on the flight home I remember looking out the window as we flew over the Thames and thinking “I never thought I’d be able to do that.” So there was no reason I couldn’t get through my last year and become a great doctor. My final year suddenly seemed like a stepping stone.
I was going to get off that plane and know that at the same time the following year, I’d be a doctor. The trip was a big confidence booster.
I had a new appreciation for the NHS too. I’m sure everyone says that, but it’s true. I don’t think you can truly appreciate the NHS until you’ve experienced other systems.
 Beyond my education, even now that I’m working as a doctor, I still draw on my experience in The Philippines. It helps me to talk to patients. Some patients have concerns about wait times and treatments and things like that, so when it’s appropriate I speak to them about how things are in The Philippines.
Beyond my education, even now that I’m working as a doctor, I still draw on my experience in The Philippines. It helps me to talk to patients. Some patients have concerns about wait times and treatments and things like that, so when it’s appropriate I speak to them about how things are in The Philippines.
I do my bit to try to get people to realise that the NHS is the best healthcare system in the world.
Many of the nurses who work in the NHS are from The Philippines, so that helps when I’m explaining things to patients. I even met a nurse who gave birth to her children in the hospital I undertook my placement in!
When she told me, I said I’d seen the OBG department over there with my own two eyes. She said she hadn’t realised that things could work differently until she’d been to the UK.
Having said that, the staff in The Philippines had insight into how things could be done overseas. Some staff would ask how we did certain procedures back home. I’d tell them that we did it completely differently from how they were doing it. And they’d say, “I bet you’ve got machine X and use procedure Y”. They’d be right a lot of the time.
Many of the staff have been to private hospitals in The Philippines, so they know how much better things could be. But even so, our public hospitals are better still than many of the private in The Philippines.
If a patient passed away in The Philippines, staff would sometimes ask “Do you think that patient would have lived if we were in the UK?” and oftentimes the answer was yes. That was difficult.
 So, you’re now in FY1.
So, you’re now in FY1.
I am, yes.
So could you explain, for those who might not know, what exactly is FY1?
So FY1 is your first year out of med school. First, you do FY1 and then you do FY2, and over those two years, you do six different jobs.
Each job is 4 months long. There’s quite a competitive process towards the end of 5th year, but I was lucky enough to get my first choice in the job I wanted to do. I’m currently working at St. James’ Hospital in the elderly department. I work with lots of lovely old people, and I love it.
FY1 doctors are the most junior doctor on the ward. That means we have the pleasure of doing a lot of the menial tasks like taking blood, putting cannulas in, doing prescriptions, writing notes (lots and lots of notes), and then there are all the forms and other bits of admin.
But sometimes, we’re the only doctor around. And sometimes, when there are acutely unwell patients, we’re the only people there who can do anything about it. So we flit between doing bits of everything, keeping things ticking over, to suddenly being expected to manage a seriously unwell patient.
It’s just one big learning experience.
Sometimes it feels a bit like when you pass your driving test. As soon as you start driving on your own, you realise the lessons meant nothing and you don’t know how to drive at all.
 But we still have to get a lot of things signed off. We have to write up our reflections, and we have to have in-depth discussions, and then there’s the training. Lots and lots of training and teaching. But it’s good to be on the job and get paid for what we’ve always wanted to do!
But we still have to get a lot of things signed off. We have to write up our reflections, and we have to have in-depth discussions, and then there’s the training. Lots and lots of training and teaching. But it’s good to be on the job and get paid for what we’ve always wanted to do!
You used the driving test analogy, which helps highlight the fact that medicine is all about the experience. Do you think that your time in The Philippines contributed to your success in FY1?
Going there, alone, travelling, meeting new people, and being out of my comfort zone — these are the things I draw on.
Spending time in The Philippines made me feel like I can do things that I’m scared of. I’m now in situations where I’m out of my comfort zone every day. I just think to myself, “Well I did it then so I can do it now.”
So looking to the future, what are your ambitions?
Well I know I don’t want to do surgery! But I’m interested in anaesthetics and A&E. I spent time in those areas while I was out in The Philippines, and I’ve continued to enjoy them at work.
I’m thinking of going down the hospital-based medicine route. Maybe acute anaesthetics and the emergency side of things. But I also really want to get involved in medical education. I’m thinking about taking a year out after FY2 and doing a job that involves teaching medical students.
 What words of encouragement do you have for the person who is thinking about undertaking a placement like this, but might be too nervous to go or aren’t sure if the experience is for them?
What words of encouragement do you have for the person who is thinking about undertaking a placement like this, but might be too nervous to go or aren’t sure if the experience is for them?
It’s always better to push yourself to do something than it is to look back and wonder what could have been.
The potential benefits of going massively outweigh any fears you might have. I know that I surprised myself.
If you think you’re too nervous and that you’re not capable, you’re underestimating yourself. It’s impossible not to have a good time with all the staff and your housemates over there.
And if you could sum up the experience in a word, what would it be?
That’s a tricky one. I think probably “inspirational”.
Read more about our medical electives in Iloilo.

MEDICAL
ELECTIVES
To start customising your own overseas experience, head to our medical electives page using the button below.
To start customising your own overseas experience, head to our medical electives page using the button below.