Jack undertook his dental elective with us in Peru in 2017. He talks about his experience below.

I knew I wanted to be a dentist when I was about 13. It was between medicine and dentistry, but dentistry tipped it for me because it seemed like it was going to be more hands-on and utilises hand motor skills.
Another factor that appealed to me was that it was a career that encouraged lifelong learning and allowed me to help patients daily.
I went to Plymouth Peninsula Dental School, which is a fantastic modern Dental school which equipped me well for the working world. I was introduced to one student who was a few years ahead of me and had done an elective with Work the World. I knew I wanted to do something like that, so I reached out to her and asked her if it was worth doing.
She said yep, do it — Work the World is fantastic. I chose to travel to Peru because I’d never been to South America and thought it would be fun to learn some Spanish. And before I knew it, I was on a plane to Arequipa.
I was doing weekly Spanish lessons in the run-up to the trip, but I wasn’t sure how proficient I was going to be by the time I travelled. I also learned that several people in Arequipa spoke Quechua, the language of the Inca.
So, I developed a visual communication aid to help me with diagnoses and to help provide preventative advice.
For example, I had a pain scale that had images to denote the kind of pain a patient might be in. I had a picture of pins they could point to if the pain was sharp. Or there was a picture of an ice cube if the pain was triggered by anything cold.
The preventative advice section had pictures of things like sweets, biscuits and chocolate so I could effectively ask “Are you eating any of these?”
There’s been a big shift in dentistry in the last 50 years, especially in Europe. Dentistry is no longer reactionary — it’s a lot more about preventative treatment. I found that when I was in Arequipa, there wasn’t much in the way of education about what causes tooth decay and gum disease. Few people were being told to cut out the sugars, brush twice a day, make sure their fluoride exposure is high and so on.
So, the communication tool I made was incredibly helpful.
My University helped me by producing the finished product, so it was quite a professional-looking booklet. It was a bit like a flow chart, functionally. From a preventative education perspective, it was invaluable. I got the sense that talking to patients about what causes tooth decay was eye-opening for them.
Was it just a general lack of awareness you feel was contributing to the severity of the cases you saw? Or do you think it could also be resource related? For example, people eat cheaper, more sugary foods in absence of anything else.
There was a high availability of refined sugars. I remember there being a popular soft drink called Inca Cola that was a sort of fluorescent green colour and undoubtedly full of things that aren’t good for you.
Having said that, even in the UK people don’t necessarily understand that a lot of pre-made sauces, like ketchup, have a lot of sugar in them.
There’s always room for a bit of education in these things, and that has been a really important shift in medicine and dentistry.
Were there any demographics that you noticed were more affected by this than others? I’ve spoken to people before who’ve noted that in some countries decay is far worse in younger people.
Well, I did spend some time in a juvenile detention centre. That was the one place I couldn’t use my communication tool as we were patted down and had to hand in all our belongings before heading further into the building.
It was a fascinating experience and very different from the UK. The dental chair was powered by a petrol generator, which made conversation quite difficult.
We saw kids from the ages of probably around 12 to 16. The coordinator for the detention centre would bring in five patients at a time, and we had two chairs operating simultaneously.
These kids had a lot of decay. They needed four or five fillings each. My supervising dentist and I spent the whole day removing tooth decay and placing fillings.
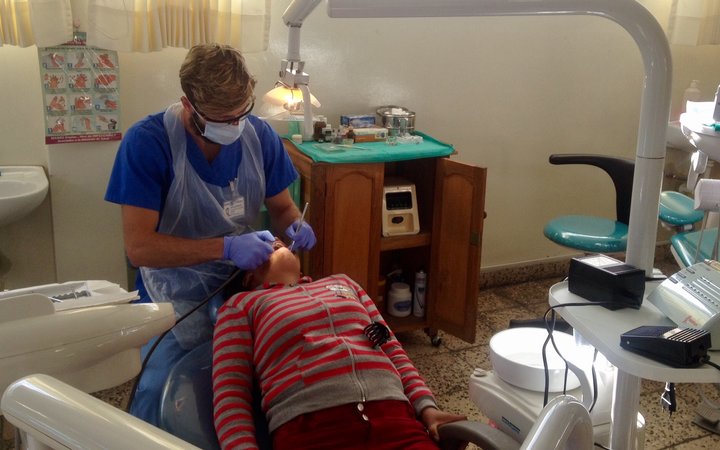
— See what it's like to practice in a low-resource healthcare system —
Though I don’t know whether or not this was more to do with diet in the detention centre or access to things that would help with oral hygiene. To see that much decay was quite shocking, and again this highlighted to me the importance of education and preventative advice.
When I was in the outpatient clinic, where my main placement was based, I didn’t see many young people.
What was your interaction with the local dentists like?
They were fantastic. They talked me through a lot of the rationale behind why they did things a certain way. Despite any language barrier, there might have been, wherever you go in the world it’s the same profession, so we had plenty of common ground.
They took me under their wing. As I say, my Spanish was only conversational, but the local dentists were patient with me, which I appreciated. Dentistry can get quite advanced when it comes to terminology, but because most terminology is Latin based…
So, there was some universality there?
There was. There were plenty of times when the local dentists would use a Spanish term for something, and I’d understand what they meant thanks to the common Latin root of the medical term.
Were there any stark differences compared to the UK?
At university, the educational focus is on holistic dentistry, and prevention is the priority. It’s about the whole patient, not just about the mouth. So, we learn a preventative approach — sort out your brushing, sort out your diet and you’re less likely to have fillings. That means you’re less likely to need treatment in the future.
As I mentioned before, treatments in my Placement were far more reactive.
And patients had to pay the full sum for any treatment they received. If they wanted local anaesthetic, they had to pay for it. If they wanted the dentist to use gloves, they had to pay for them.
I brought all my own PPE. And at the end, I was able to donate a lot of what I brought over to them. Their resources were extremely low in that regard, at least in the government clinic I worked at.
That said, the dentists did the very best they could with what they had.It was eye-opening in the sense that it renewed my appreciation for the NHS. In the UK, we grow up thinking that yes, the NHS is fantastic, but also that it’s a human right. I think we tend to develop a sense of entitlement towards it.
Practising dentistry in Arequipa showed me that we absolutely should not take it for granted. Because one day, should the NHS come to an end for whatever reason, things could be very different for us.
I came away from the experience much more appreciative.
So, what was the day-to-day of the placement like?
In the mornings I’d get up and jump on the bus to the outskirts of the city. We were packed in like sardines, but the bus journey was an adventure in and of itself. Arequipa is a beautiful city, so it was cool just winding around the roads, watching the morning’s hustle and bustle.
Then I’d get to the clinic, say my good mornings to the staff and wait for the patients to start rolling in.
When patients came in, the local dentists would tell me what they wanted me to review and what would likely be the issue. All the charts were done on paper as opposed to the computer systems we’re used to backing home. I’d learned paper charts at uni, which they teach you right at the start just so you know what they are.
But I’ve not thought about it since, so it was interesting to have to rely so heavily on them while I was over there.
If there were any complex procedures, I’d get the opportunity to watch one of the more senior dentists go to work. There was a case of a girl who had an extra tooth. It was showing up on the X-ray as being buried under the top central incisors, which are your front teeth. If that stayed there, there was potential for it to have resorbed the roots of the other teeth. So, she could have lost those teeth altogether.
They decided to operate, so I got to observe the dentist perform the oral surgery, which was very interesting and not something I had seen at university
The X-rays, by the way, are not digital. They were all developed in the darkroom, which was interesting to see.
And then in between patients, we’d chat about dentistry and the differences between our approaches. On that point, there were some instances where I was surprised to see certain practices.

— Get to know local healthcare staff and why their practices differ —
One particular practice that differed was the mixing of amalgams. I noticed quite early on that the local dentists were hand-mixing in the mercury.
Mercury is toxic and has detrimental effects on the environment once disposed of. Once in Amalgam mercury is safe as an alloy is formed, but hand mixing is something we don’t do anymore in the UK. These were the processes and materials available to local staff and that was what they worked with.
The material selection was a big stand-out in general. In the UK, we’re so lucky that we have multiple choices when it comes to material options. Each person, each tooth, will have some uniqueness to it where you might think that a certain filling might not work in here, or that crown material might not work in there. And we can pick and choose what materials to use and when.
Whereas in Peru, this was not the case. My placement was in a government outpatient clinic and we had the resources we were given, and they were a little limited.
You were talking about amalgams and mixing in mercury. For a layperson, what is that process? What was it about the way they were working that most surprised you?
Amalgam is essentially an alloy between mercury and things like tin silver, copper powder and so on. It forms what we call an amalgam. This has been the primary filling material in dentistry for a very long time. In the UK this is being gradually phased out in favour of more advanced resins called composite fillings.
What was interesting in Peru was observing the local staff mixing amalgam by hand. Again, in the UK this is being phased out, but when we do use it, the materials come in a capsule which mixes the amalgam for you.
To mix it by hand is a real skill because you have to be incredibly careful with the ratios. That’s why the Peruvian dentists were doing it and not me!
And that’s the point of a trip like this — to see things that you just cannot see in the UK.
Absolutely.
So, you finished your placement and came back home. What was your trajectory from there on?
I got home and had two years left of uni. I finished that off and then decided to try to get a placement in my hometown. My friends and family were there, so it made sense to me. The way it works in dentistry is the NHS pay for your final year and you work solely for them for that year. It’s called a Dental Foundation Year or Dental Foundation Training.
You do one exam and two interviews, which gives you a rank among all the other dentists in their 5th year of dental school. You then choose your number one area, which for me was Cambridgeshire. There is something like 60 areas and in each are 12 - 16 practices, each with one place.
There are roughly 1300 students and around 1100 places, so unfortunately some people do not get a place. Luckily, I ranked pretty high and was able to get my first-choice area, and then within my area, I was able to get my first-choice practice. I spent the year there and completed that in August just gone. I’m still working there now as well as in another practice just outside the city.

— One of the Work the World houses —
So, what was the transition from education to the real deal like?
It’s interesting because at university you have a supervisor come and check every stage of the procedure. Then, all of a sudden, you’re by yourself and the onus is solely on you to make the right decision. Having said that, we do have educational supervisors. If I had a difficult case or something I’ve not encountered particularly frequently, I can get them to come down at which point I’ll ask them for advice. So that first year you have lots of support around.
I’m lucky enough at my practice now that if I come across a complicated case, then there are plenty of people around who can offer advice and support.
There are other things that university doesn’t necessarily prepare you for. The business side of practising dentistry and the limitations that can place on you, clinically. While we were at university, we had access to any material you could want. That was so you could get experience with it.
But what you’re not made aware of at the time is that a lot of these materials are costly, and so not available on the NHS. We still have access to lots of materials, but we have to be more conservative about what we use otherwise we’d be running our practices into debt.
If you want a denture or a crown on the NHS, it’s £269. After a root canal, often the advice is to get a crown because it’s the best way to seal the root canal and for the tooth to last longer. Not every patient is going to be able to afford that £269.
But that’s what’s great about professions like dentistry and medicine — there are always things to learn, and it never stagnates
So, ambitions for the future. Your own practice eventually?
I don’t know. Back in the day when I was young and naive, I would have said yes! But there’s so much regulation, and I’ve seen from various practice owners that they don’t have an awful lot of free time. It’s all-consuming.
And that’s fine for some people, but I enjoy spending time with family and friends. Don’t get me wrong I love dentistry, but I want to also do things other than dentistry. Also, it’s early days, so we’ll see.
At the moment my focus is on being good at my job. I’m doing lots of extra courses, trying to invest in and advance my skills so I can do the best for my patients. Job satisfaction and life satisfaction are intimately linked, and that’s why I want to continually strive for improvement and development.

— Going overseas for your placement opens up unique travel opportunities —
Another thing I’d like to do at some point is something called Mercy Ships. It’s a massive ship that travels to Africa and the Caribbean. On board, there are qualified medics, dentists… lots of healthcare professionals. They dock up for several months and provide free medical and dental treatment for patients who can’t afford it otherwise. Often it can be life-changing!
I’ve wanted to do it since my gap year, and I thought that a Work the World placement would be a good stepping stone to it. As I say, we’re so lucky over here with food in abundance, roofs over our heads and healthcare free at the point of access. It’s only fair to give back to people who haven’t had the same opportunities as those I’ve had.
Whether I want to open a practice or not? I don’t know. We’ll see what opportunities present and I’ll enjoy the process all the same
That’s right. It’s easy to become fixated on goals and miss the road you took to get there, isn’t it?
Exactly. I think just enjoy the journey, enjoy the process. University was fun, and my elective with Work the World was brilliant, now this is the next chapter and I’m enjoying that.
As you say, if you’re doggedly pursuing a goal, there’s always another goal after that.
Dentistry, thankfully, is a very stable job, so I don’t have any concerns on that front either.
What has that been like if you don’t mind me asking?
It has been interesting! So, it all kicked off in March and obviously, we weren’t able to do any treatment as we were closed. There were exceptions, so if you were a designated urgent dental care centre you could treat certain patients. The NHS wasn’t offering up much funding for this, but my boss wanted our practice to become an urgent dental care centre so we could provide for patients who were in severe pain.
In reality, it meant triaging lots of patients. I was on the phone every day, which was surprisingly tiring. I have an even greater level of respect for our reception team after that experience.
Mostly I just felt for our patients. For some of them, their problem was minor — they’d lost a filling and were in no pain. For them, the advice was to keep the area clean and monitor it for any changes.
On the other hand, some patients were in incredible pain. All we could do was prescribe painkillers, and antibiotics where appropriate. It was a challenge because you get into the profession to be able to help people. So, to sit on the phone and not be able to do anything was frustrating.
Thankfully, because we became an urgent dental care centre, we were getting lots of referrals from places outside our practice area. You know, patients with severe swellings in serious pain that couldn’t be managed by anything we could prescribe. To begin with, all we could offer was extractions, which today sounds a little extreme given that it’s typically a last resort.
But then once we started getting in all the appropriate equipment and PPE, we were able to expand into root canals and other treatment options.
Now, we’re fully open again. We’ve got these giant masks on our faces, and gowns. We stagger patients too, which means we can see fewer in a day than we typically would.
I’m guessing there’s a significant backlog as well. You must be on the back foot.
I’ve only just finished treatment for most of my patients whose appointments were cancelled during the lockdown. In our practice, we brought our emergency cases in first, then patients who had open courses of treatment, and I’ve only just started doing exams again. Even then they’re quite limited in number.
The other problem is that I’ve had kids with lots and lots of decay, and they’re maybe three years old. They’ve developed abscesses from decay that hasn’t been able to be treated over lockdown, so I try to refer them to the hospital for treatment under general anaesthetic, as they’re too young to be able to treat in surgery. The problem is the hospitals have an enormous backlog of patients needing surgery, which means none of the paediatric surgery lists is open for 6 - 12 months. This has made things quite difficult, as you can imagine.
The pandemic has had a knock-on effect that I don’t anticipate we’ll ever be able to accurately measure.
That’s right. And we’re not going to be back to normal service for quite some time.
So to round things off, if you were to have a conversation with someone who was perhaps hesitant to undertake an elective placement, what words of encouragement might you offer them?
I’d just say that I had the best time.
I was slightly apprehensive about going out. I was going by myself and was planning on doing a little solo travelling after the placement itself. The fact that I was headed to South America — somewhere I’d never been — added another element to it.
But it was fantastic. The Work the World house was brilliant, there were 34 of us in total. I was the only dental student, but the rest were medics and nurses who came from the States, the Netherlands, Australia… We had this camaraderie that can only be borne of being thrown together like that.

— Meet healthcare students from all over the world and make lifelong friends —
So, there was that support network. But then you also have all the Work the World staff, including the catering team who cooked us amazing food every day. The other staff are there to check in with you and make sure you’re alright.
If you’re feeling apprehensive about it, all I can say is don’t worry. You’re going to make lots of friends. I still stay in contact with lots of people I met out in Peru.
And then there’s the experience you get clinically. It just opens your eyes to other ways of approaching treatment. You’ll also see things you would never see in the UK.
Just go for it, don’t think too hard about it. Take the opportunities while you have them because once you’re working it’s not so easy.
I did look into some of the other companies offering elective placements, and Work the World was a little pricier, but I can tell you that is 100% reflected in the service you get before you travel and while you’re overseas. The support and facilities are brilliant.
We bumped into some medics who were with another company and they said it was the worst thing ever. Nothing was organised, they had to fend for themselves when it came to food and all the rest. Because we didn’t have to worry about that, we could focus on our placements and enjoy ourselves out there.
I fundraised my placement costs using GoFundMe. I set up a page, told people what I was up to, explained why I thought it was a worthwhile trip, and managed to fund the whole placement in two weeks. I tried to incentivise people to donate as well, so if you donated over £100, you got an electric toothbrush. Just little things like that.
If you’re worried about finances, and I know I was when I was a student, there are always ways to get funding. I even managed to get some money from the university to help me get out there.
I would 100% recommend Work the World to anyone.

Want to
Travel?
Want to go an overseas dentistry elective like Jack? Check out our dentistry page below find out about the amazing opportunities on offer.
Want to go an overseas dentistry elective like Jack? Check out our dentistry page below find out about the amazing opportunities on offer.