Dundee University 2020
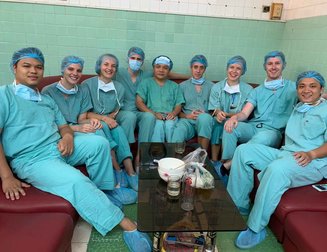
For me that moment of knowing, that I was ready and worthy of a job as a junior doctor in the NHS, came while I was saving lives with other surgical interns in Vietnam.
I really liked the sound of Vietnam, a peaceful non-English speaking country in Southern Asia, surrounded in history and culture. It would be huge step out of my comfort zone; I would be practising medicine in a totally different healthcare setting, and so I figured I should opt for a more practical surgical placement that relied heavily on observing and mirroring procedures rather than through verbal conversation.
I have always had a passion for gastroenterology and abdominal surgery, so I could not believe it when the fabulous team at Work the World offered me the opportunity of 6 weeks in the digestive surgery department.
I was also secretly keen to avoid the typically popular elective destinations such as Australia and New Zealand with traditionally more wealth than rural Asia. My objective was to hone my knowledge and practical skills to a standard where I felt confident, I was ready for life as a future NHS doctor. I felt it was important to prove that I could still perform comfortably without relying on fancy equipment, readily available radiological investigations, or reliable internet connection.
The whole process of enquiring and organising was so easy. The WtW website was easy to navigate, and the team were quick to respond to my enquiry – they phoned me back the same day and the whole thing was outlined in a matter of hours. My placement, my accommodation, catering and my visa were all sorted for me, leaving me to book flights and insurance. It was reassuring to know the prices of the placement did not vary the closer it got to the date of travel. Very handy if arrangements change at the last minute. The team also reassured me that the placement supervisors were incredibly flexible, so if while I was there, I decided after four weeks I wished to switch from general surgery to another specialty, I could do so.
It was a very surreal experience to be guided around the hospital in Hue. It felt very crowded and industrious. The roads leading to the hospital were also very busy with the motorbike being the most popular mode of transport in Vietnam. There was a huge number of patients in the waiting room for the non-emergency open clinic, each accompanied by family. It was interesting to observe the on-the-day appointment system, where the patients had to queue for hours and hours before being seen. I was also very aware on my first few days of how hot it was, how most buildings had their doors and windows permanently open and the distinct lack of ventilation on most wards. I was also pleasantly surprised to see so many young local medical students hanging around the ward, eager to learn and keen to introduce themselves to us. All were very friendly and keen to practise their English with us. On my first day I was also introduced to my clinical supervisor and four other medical students from Germany who were also on their electives in the department.
While on placement, I was under the supervision a surgical consultant, an attending in Digestive & Abdominal Surgery and head of department. As part of my surgical placement, we were encouraged to fully immerse ourselves in the role of trainee surgeons. The consultant would dash between patients, asking us to examine the patient and present the case before being quizzed on the theory. Like the teaching partnerships in the NHS in the UK, each surgical consultant here is paired with a surgical resident. Our resident was someone closer to us in age and in-tune with our own learning requirements. He was very approachable and would often explain what was happening during procedures if the consultant was busy. During operations, once the consultant had finished, removed his scrubs, and left, it would be the job of the resident and I to close the skin wounds. It was here where I would be instructed on the Donati suturing technique, more commonly known as the vertical mattress stitch, named after the Italian surgeon from the early 20th century Mario Donati. This made the placement more enjoyable for me as I was treated as an equal team member. Common operations we would see included total gastrectomy’s for stomach cancer, colectomies for colon cancer, bile duct stone removal, haemorrhoidectomies, anal fistula repair and Whipple’s procedure for pancreatic cancer.
As a core member of the team, I was expected to be present for the same hours as those working at the hospital. This meant waking at 05:30 every morning, getting a motorbike-taxi into the city centre ready to start the morning ward round at 07:00. I would be invited to join the whole department for a meeting at 07:30 for a discussion of the day’s cases and establish where each consultant would be based in the hospital that day or if they would in fact be stationed at one of the other two hospitals in the city.
At 08:00 the consultant would take us for coffee while the patient was prepped by the anaesthetic team, before finally we would get changed and scrubbed to commence the procedure at 08:30. We would work until midday where the culture of Vietnam is to travel home for an extended lunch break and spend two hours with the family. At 14:00, we would reconvene and begin either the afternoon operation list or hold clinic. Here, patients would attend for a consultation or for further investigations as part of their operation planning. We would finish after 17:00 most days. It was an intense lifestyle. Long hours in high heats and poorly ventilated operating rooms made for a physically challenging day-to-day routine and I often found myself in the first week longing for a comfort break to take on water or iced tea. Fortunately, I found myself acclimatising over the following weeks and the comfort breaks would be more and more infrequent until the point where I did not need to take any. I had mastered my routine and knew exactly what and when to eat or drink so that I was consistently performing at my best, or as they say in Vietnam, “trăm phần trăm!”
A healthcare placement will be whatever you make it, but I think there is something to said for the accommodation and living arrangements in between shifts. The Work the World house in Hue was a beautiful cottage situated away from the busy city, by the Perfume River which made for a scenic walk home at the end of the day. The house team were all so kind and personable, they were genuinely interested in your day and always went the extra mile to make your stay more comfortable. I felt clean, safe and well fed.
My surgical supervisor made clear to me that he expected me to attend the hospital every week Monday to Friday, but he strongly encouraged me to use the weekends to travel and see more of his beautiful country. I am so glad I did, because one forgets that they are in a foreign country and the mistake would be to spend all day inside an operating theatre. By using public transport, I immersed myself in the culture, I visited nearby towns and cities, I tried the local cuisine and made sure to photograph the most popular tourist spots that the country had to offer. The WtW house staff were very helpful with facilitating these trips, providing us with recommended travel companies as well as a journal of previous visits by other elective students with favourite locations such as Hoi An, Da Nang & the Dragon Bridge, Phong Nha Ke-Bang National Park home to the numerous caves, as well as the two traditional capitals Ho Chi Minh city and Hanoi.
It is hard to believe for the whole six weeks I did not ever feel alone, which can be a common and scary possibility for a solo traveller in a non-English-speaking country. Throughout the placement, you have both a clinical contact who provides you with one-to-one supervision while at the hospital, and a programme manager at the Work the World house. Both were always on hand to answer any queries or to make minor changes to my placement. They are also there for pastoral support if you are having personal struggles while on placement or just missing home. You also have a family of companions living with you in the Work the World house to eat dinner with or watch a movie. It is so important as a healthcare professional to be able to switch off from work, and having other elective students there made that so much easier. You really do make friends for life.
If I were able to pass on one piece of advice to my peers on elective is to make friends with either the local medical students in your department or indeed other interns on placement there. The four final year medics I befriended from Germany were my family. We all started in general surgery, but they had organised time in anaesthetics, plastics, orthopaedics etc. so although I didn’t see them during the day, we all met up in the evenings. Often we would go for a drink, but sometimes we even went bowling, karaoke singing or to the cinema. I felt like I had known them for years. This made travelling at the weekends much easier and enjoyable. We would talk about our cases from that day, about our different healthcare systems back home, we would joke and tell stories of our time as medical students. One day we hired motorbikes and drove to the coast and spent the day at the beach.

It was fascinating to experience the surgical world of the hospital in Hue. In my placement hospital, it felt like I had time-travelled back to the mid-20th century of the NHS. I recognised the equipment and the techniques, but they felt out-dated. Old laparoscopy machines, reusable fabric gowns, one size of sterile glove, old creaky wooden doors and vastly different practices surrounding hygiene and sterility. A lot of conversation amongst my fellow interns during down time revolved around under-funding and health insurance. It really brought home how fortunate patients are in the UK, with a free National Health Service at the point of use. It appeared the wealthier patients sought screening for symptoms earlier at a more modern international hospital, where a great number of clinicians were either English-speaking or indeed from English speaking countries. This left many Vietnamese nationals without health insurance to suffer their ailments for longer, until too late a stage where management was no longer curative but palliative.
The procedures undertaken in Vietnam are not unlike those in the performed in UK. I can, however, say with some confidence that the number of gastrectomy’s for diet-related stomach cancer is far greater. Worldwide, stomach cancer is the 4th most common malignant disease. In the UK, however, it is the 17th most common type of cancer with only 6,000 people are diagnosed with stomach cancer every year. Compare this to the 55,000 cases of breast cancer in women and 45,000 cases of prostate cancer every year in men. Hemicolectomy’s or anterior resections were other procedures which I became familiar with on theatre lists as, again, colon and rectal cancer is a common problem in Vietnam. My understanding for this phenomenon is a result of the lack of screening in Vietnamese healthcare. A greater number of cases are discovered too late and early preventative measures are no longer adequate, thus surgery is the only remaining option.

As these patients often had late stage disease, and their conditions more complex, it meant that there were a greater number of patients crammed on to the ward and thus less time spent seeing each patient. It was staggering. A lot of the basic patient care was performed by the family members which made the wards even more overcrowded. The surgical nurses spent their days dealing only with wound dressings and intravenous drips. This worried me as my thoughts immediately turned to post-operative complications and detecting early signs of sepsis.
As a result of this underfunding, staff were constantly vigilant about saving resources which often translated as there was no room for error. For example, surgical procedures were carried out without regular swab checks from the scrub nurse. Only five swabs were allocated to each operation and thus the surgeon could not afford to leave the rag in the abdominal cavity by mistake as they had to be washed, sterilised and re-used for another case. Sharps were disposed of in a standard general waste bin rather than a dedicated sharps waste bin because they could not afford to have a separate waste bin. They also could not afford a red kidney bowl to hold sharps safely when not in use, thus putting the surgeon and the team at higher risk of sharps-related injury. Patients were not given identifying wristbands because they could not afford to spend money on that luxury. They could not afford to operate on the wrong patient. I do not use the phrase “couldn’t afford to” simply with regards to cost, but instead on a deeper level alighting to the fact that there was no room for error. The staff in the hospital were super humans who had to get it right every time. I compare this mindset and attitude to a farmer who carried the weight of a buffalo in bags of rice on the back of his motorbike in a t-shirt and shorts without a safety helmet and navigating the chaotic traffic system without injuring himself or his precious cargo – he could not afford to make a mistake. Simple.
I relate this back to how this could influence my practise as a junior doctor in the UK. I look at all the safety nets our healthcare system has in place and in a way, it is disheartening to see the UK to be so lazy and accident prone that we need a safety barrier to lean on. We can afford to make mistakes. This is a depressing and shattering revelation, but if you look under the surface, you may come to accept it to be true. You can study textbooks endlessly until you think you are as prepared as is physically possible, but there must be something in either our primary or secondary education system where we are not taught to take responsibility for our life choices early enough in our careers. We stumble through medical school and come out of the end of it and we have not harmed a patient and we evaluate this to be a success. But the reality is it only leaves the space for damage to be done later down the line when for example, we are the only doctor working in the hospital on a busy night shift.
It was a Vietnamese tour guide who told me a story about how proud the Vietnamese people are, and I relate it somewhat to this discussion. When one sets out to accomplish a task, yes it may seem difficult, but if one tackles the same challenges every day, then come the new dawn the experience has not been wiped from memory but rather an opportunity for one to build upon. Overtime, the problem appears less troublesome as the individual masters the skills which allow him to tackle the problem. In the developing country of Vietnam, where overpopulation is a major issue, the Vietnamese people are faced with daily challenges which shape their lives. Individuals must be able to adapt quickly and master a wide range of core skills to survive. Whether it be farming a sugar cane crop, cutting and harvesting the crop, transporting the product on busy and crowded highways while balanced precariously on a motorbike, to finally sell the product in order to make enough money to purchase for the large family at home. In Vietnam, nothing is easy and lots of hard work and physical effort goes into making a living. These are not always intellectually challenging tasks, but nonetheless they remain physically arduous and individuals must remain mentally resilient. As mentioned, the income is spent on food for the family. It is no surprise that malnutrition is still common in most provinces and life expectancy and infant mortality rates are stagnating.
A parent’s child is the driving force for his efforts. They are the future of the bloodline and of the country. It was the vice-rector monk at a Buddhist temple in Hue, who taught me “as luxuries are not sought after – they are not missed.” Expensive items are often not necessities. If you remove the desire for many unnecessary belongings, what remains are family, your love for them, the happiness created from the memories with them, and finally the knowledge & skills by which you can provide for them.
Vietnam has taught me that I can always be better. The medical student I was when I passed my finals last year, simply was not good enough to survive in the big bad world of foundationship years come graduation in June 2020.
I remember a time when I had only been at university for a few weeks and I asked a senior medical student during a tutorial, “at which point do you feel like you are ready?” The fifth-year student smiled and knew instantly what I meant, and his answer sounded well-versed and considered. His reply was along the lines of “…you don’t really notice at the time, but one day you’ll be working on the ward or teaching in a tutorial and your mind casts back to how far you’ve come since fresher’s week and you can see an obvious difference from the individual you were then to the soon-to-be doctor I am now. That act of comparison between the past and present is the moment you know you are ready, worthy prepared etc.”
It was everything I had hoped to be when I started medical school. I was proud of the responsibility and of our achievements as a junior surgical team.
Read more about our Electives in Asia, where you'll discover a variety of options, in Vietnam and other exciting countries across the continent.